Welcome to About This Word, where Wordsmyth showcases commentary about relevant words in the news and media our users and staff find interesting. Today’s word: “opioid,” written by Wordsmyth science writer Andrea Hazard.
What Is An Opioid?

The term opioid is derived from the root word opiate . When the term originated in the 1950s, it meant a substance with opium-like properties. The definition has since been refined to “a substance that is able to bind the opioid receptors.” Opioids include natural, synthetic, and semi-synthetic compounds (1). The term “opiates,” however, refers only to natural opioids.
A receptor protein triggers a cellular response when a small molecule called a ligand binds to an opioid in the nervous system (2).
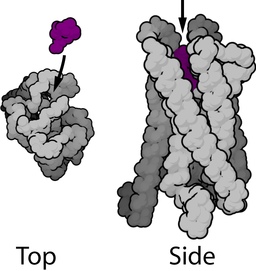
The Mu Opioid Receptor
Activating a particular opioid receptor, called the Mu (µ) receptor, results in pain suppression and a feeling of euphoria. The Mu receptor is activated by dopamine, a substance naturally produced by the body. But other substances can activate the Mu receptor as well, including morphine. Heroin and many prescription opioid pain relievers are metabolized into morphine in the body. (3)
Physical Tolerance and Addiction
Evidence indicates that mammals, including humans, naturally produce trace amounts of morphine. (4) Prolonged exposure to high morphine levels, which can occur during prescription or illicit drug use, can lead to physical tolerance, which reduces the drug’s effectiveness as the body physiologically adjusts to the higher levels present. Therefore, when physical tolerance occurs, a higher dose of drug must be administered to achieve the same effect. (5)
Tolerance can lead to physical dependence, a state in which a person suffers symptoms of withdrawal if drug use is discontinued. These symptoms include irritability, sweating, nausea, and vomiting, when drug use is discontinued. Physical tolerance can then lead to addiction. (5)
Concerns About Addiction
Physicians have long been aware of the addictive properties of opioids. During most of the twentieth century, opioids were reserved for the treatment of cancer pain and other acute pain, as well as for anesthesia. However, physicians became increasingly concerned about the inadequate treatment of chronic pain, a pervasive problem that, according to the World Health Organization, afflicts up to 22% of patients seeking treatment in primary care facilities. (1)
In 1980, concern about chronic pain was increasing. A letter in the New England Journal of Medicine reported that out of 11,882 patients who received narcotic drugs, only four became addicted who had no prior history of addiction. A subsequent 1986 study concluded that only two out of 38 patients receiving long-term opioid treatment became addicted to opioids. Those two patients had a prior history of addiction. (1)
Many physicians concluded that the benefits of using opioid painkillers to treat chronic pain outweighed the risk of addiction, and as a result prescriptions for opioids grew by 533% from 1997 to 2005 (5). So began the opioid epidemic. (1)
The Opioid Epidemic
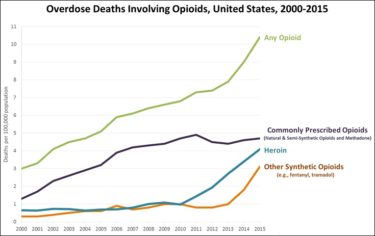
According to the National Institute on Drug Abuse, 21-29% of patients who use opioids to treat chronic pain develop an opioid misuse disorder. An estimated 4-8% of patients who misuse opioid painkillers transition to heroin. (6)
The rise in heroin use has been particularly steep since 2010. Possibly, this is because prescription opioids have become more difficult to obtain due to stricter prescription guidelines, and due to the fact that addicts cannot get the same feeling of euphoria from extended release tablets that were introduced around this time to stem the epidemic. (4)
For more information please visit the following websites:
American Society of Addiction Medicine
National Institute on Drug Abuse
References
(1) Wilkerson, Richard Gentry, et al. “The opioid epidemic in the United States.” Emergency Medicine Clinics 34.2 (2016): e1-e23.
(2) Al-Hasani, R., & Bruchas, M. R. (2011). Molecular mechanisms of opioid receptor-dependent signaling and behavior. Anesthesiology: The Journal of the American Society of Anesthesiologists, 115(6), 1363-1381.
(3) Inturrisi, C. E., Schultz, M., Shin, S., Umans, J. G., Angel, L., & Simon, E. J. (1983). Evidence from opiate binding studies that heroin acts through its metabolites. Life Sciences, 33, 773-776.
(4) Grobe, N., Lamshöft, M., Orth, R. G., Dräger, B., Kutchan, T. M., Zenk, M. H., & Spiteller, M. (2010). Urinary excretion of morphine and biosynthetic precursors in mice. Proceedings of the National Academy of Sciences, 107(18), 8147-8152.
(5) Cahill, C. M., Walwyn, W., Taylor, A. M., Pradhan, A. A., & Evans, C. J. (2016). Allostatic mechanisms of opioid tolerance beyond desensitization and downregulation. Trends in pharmacological sciences, 37(11), 963-976.
(6) A subset of people who abuse prescription opioids may progress to heroin use. (December 2015). Retrieved September 23, 2017, from https://www.drugabuse.gov/publications/research-reports/relationship-between-prescription-drug-abuse-heroin-use/subset-users-may-naturally-progress-rx-opioids-to-heroin.
(7) Mars, S. G., Bourgois, P., Karandinos, G., Montero, F., & Ciccarone, D. (2014). “Every ‘never’ I ever said came true”: transitions from opioid pills to heroin injecting. International Journal of Drug Policy, 25(2), 257-266.
